Diabetes changes how your body uses sugar for energy. When your body doesn’t produce enough insulin — or can’t use it effectively — blood sugar levels rise. Over time, high blood sugar can affect your heart, kidneys, eyes, nerves and blood vessels.
The good news? With early testing, the right education and ongoing support, many people living with diabetes manage it well and enjoy full, active lives. We’re here to help you do just that.
Diabetes basics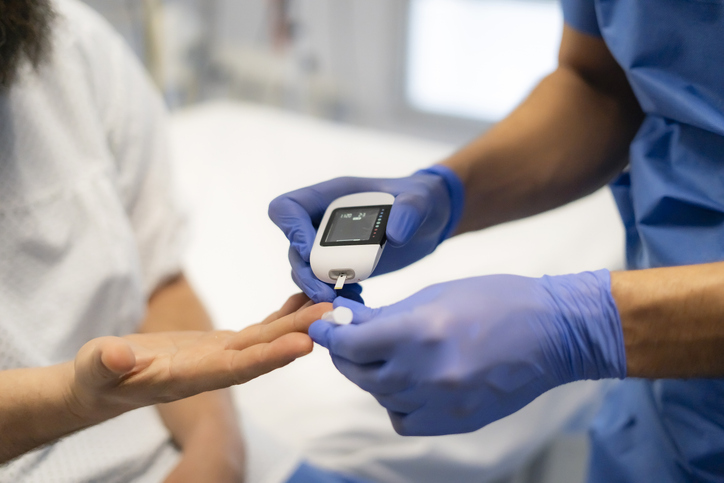
Diabetes is a long-term condition that affects how your body manages blood sugar levels. Some people don’t produce insulin at all; others may produce it but their body doesn’t use it efficiently. When that happens, sugar builds up in the bloodstream and can lead to health problems if it’s not treated.
In the U.S., millions of adults live with diabetes, and even more have prediabetes, a condition where blood sugar levels are higher than normal but not yet in the diabetes range. Prediabetes often shows no symptoms, which makes regular screening important. Catching it early can help prevent or delay diabetes.
Whether you’re newly diagnosed, at risk or supporting someone you love, we’ll help you understand what’s happening and take steps that fit your lifestyle.
With the right care and lifestyle changes, many people successfully manage it — and some people with type 2 diabetes may even achieve remission.
Types of diabetes
Type 1 diabetes
Type 1 diabetes occurs when the immune system attacks the cells in the pancreas that produce insulin. People with type 1 need daily insulin to live. It often begins in childhood, but adults can develop it too. While the exact cause isn’t fully understood, genetics and environmental factors may play a role.
Type 2 diabetes
Type 2 diabetes is the most common form. The body becomes resistant to insulin, and over time the pancreas can’t keep up. Risk factors include excess weight, limited physical activity, family history, being 45 or older and a history of gestational diabetes. Because type 2 diabetes can develop gradually, routine screening is especially important.
Gestational diabetes
Gestational diabetes develops during pregnancy when hormonal changes interfere with how the body uses insulin. It usually goes away after delivery but increases the risk of developing type 2 diabetes later in life. We work closely with expectant parents to monitor blood sugar levels and support a healthy pregnancy.
Symptoms of diabetes
Some signs of diabetes are easy to spot. Others are subtle and easy to miss. If something doesn’t feel right, it’s worth checking in with your provider.
Common symptoms include:
- Increased thirst and frequent urination
- Unexplained weight loss or increased hunger
- Fatigue, headaches or irritability
- Blurred vision
- Slow-healing cuts or frequent infections
- Tingling or numbness in the hands or feet
- Dry, itchy skin or recurring yeast or urinary tract infections
Very high blood sugar can cause nausea, vomiting, stomach pain and fruity-smelling breath. These may be signs of a serious condition that needs immediate care. If you notice these symptoms, call 911 or seek urgent medical help.
How we diagnose diabetes
We use simple blood tests to check your blood sugar levels. Your provider may repeat a test to confirm results unless symptoms and levels clearly point to diabetes.
Common tests include:
- A1C, which shows your average blood sugar over the past few months
- Fasting blood sugar, measured after not eating overnight
- Glucose tolerance testing, which checks how your body handles sugar
- Random blood sugar testing, used when symptoms are present
Finding prediabetes early gives you a chance to make changes that can slow or prevent diabetes. Starting treatment early can also lower the risk of long-term complications.
Care that fits your life
Managing diabetes doesn’t mean doing everything perfectly. It’s about building steady habits that work for you.
We focus on practical, everyday steps like:
- Nutrition: Balanced meals with vegetables, lean protein, whole grains and healthy fats
- Movement: Regular activity, like walking, plus strength training
- Weight management: Even modest weight loss can improve blood sugar control
- Sleep and stress: Small improvements can make a big difference
- Avoiding tobacco: Quitting lowers the risk of diabetes-related complications
Treatment depends on your type of diabetes and your goals. Some people need insulin. Others manage diabetes with oral medications, injectable therapies or lifestyle changes. We’ll help you understand your options and choose what makes sense for you.
Looking for extra support? Our Get Healthy, Live Well classes offer diabetes education classes and support groups that provide practical tips on nutrition, physical activity and building healthy habits that last. These community-based programs are designed to help you take small, steady steps toward better health — and they’re a great resource for managing diabetes or preventing it from progressing.
Learn more at tanner.org/classes-and-events.
When to reach out
Call your provider if you notice new or worsening symptoms, frequent high or low blood sugar readings, or signs of infection that don’t improve. For emergencies like chest pain or severe shortness of breath, call 911.