How do you launch a successful open-heart surgery program?
Same way you get to Carnegie Hall: Practice, practice, practice.
Thursday morning, the team at
Tanner Medical Center/Carrollton ran through a series of scenarios to find — and fix — any weak points in their open-heart surgery process before the program officially launches next week.
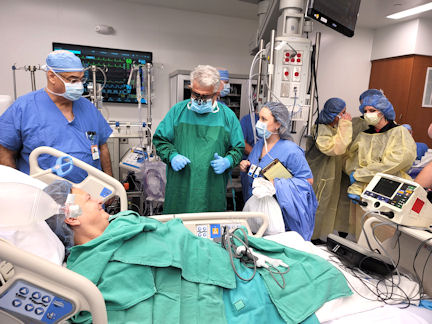
Two volunteers from the community — Anna Valve (Mimi Gentry) and Charlie Cabbage (John Crosby) — stood in as patients and moved through the process from registration all the way through open-heart surgery and recovery in the intensive care unit (ICU).
Crosby’s Cabbage — CABG is the acronym for coronary artery bypass grafting and the most common open-heart procedure — was a stand-in for a heart catheterization gone south.
“If we identify patients with advanced cardiovascular disease who require surgery or if a scenario arises where surgery is needed emergently, we can move from the cath lab to the cardiothoracic operating suite and surgically repair it,” said Christopher Arant, MD, an interventional cardiologist with Tanner Heart & Vascular Specialists who participated in Thursday’s exercises. “Another benefit of having open-heart surgery on-site is that it allows us to do more complex and technical interventional procedures because we have surgical backup.”
In Crosby’s scenario, the procedure to clear a blockage near his heart resulted in the need for surgical support. Though rare, that’s now a service available at Tanner.
That gives physicians — and patients — more options when it comes to treatment.
“We don’t have to send the patient outside of our region for heart procedures that we can perform here,” said Dr. Arant. “We have more options.”
In this scenario, when the issue was discovered, Dr. Arant called in Omar Lattouf, MD, the health system’s new cardiothoracic surgeon.
After a quick consultation, Crosby was moved from the catheterization lab table to a gurney and took a quick elevator ride down to the hospital’s new cardiothoracic surgery suites.
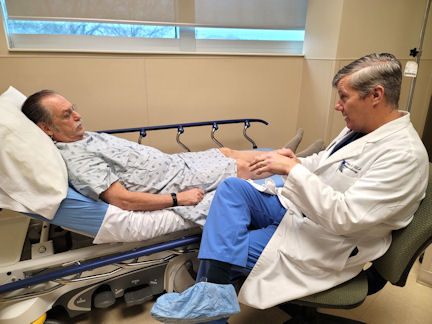
In the operating suite, staff again walked through the scenario of getting the patient ready for surgery, though Dr. Lattouf was able to stop just short of the scalpel.
Meanwhile, in the ICU, Gentry’s Valve was decompensating following a scheduled open-heart case that morning. That brought Dr. Lattouf swiftly to Gentry’s bedside, where it was determined another trip to the operating room was in order.
The scenarios allowed staff to see the different circumstances that could lead to an open-heart case, both planned and emergent.
“It’s no easy feat,” said Dr. Lattouf. “Everything must be in order. The equipment has to follow the patient through the facility, the staff has to be able to communicate and hand-off responsibility seamlessly, everyone has to know their roles — even the computer system has to work right so everything can be documented and providers have the information to make the best decisions.”
The dry-run comes after weeks of training sessions and seminars with the clinical teams that will be part of the open-heart program. Staff from all parts of the organization have streamlined the process to make sure the hospital is ready on Day One.
For Crosby — himself a real-life Tanner heart patient — being part of the practice run provided a comfort.
“We’re so lucky to have this here, and we’re so lucky to have the doctors and the staff who take this so seriously,” he said. “This is going to help so many people — and not just the patients, but their families. It’s great to see that everyone here is committed to doing this right.”
After the drill, the patient care teams came back together to discuss how things went and what they’d found as they moved through the day.
Improvements will come fast: The program starts Jan. 24.
More on the heart services at Tanner Health System can be found at
TannerHeartCare.org.